Putting an end to pay and chase
Governments can take a proactive approach to fraud
By Jon Lemon, Solutions Specialist, SAS
The words “government” and “fraud” can be found in countless headlines. But it doesn’t have to be the case. Sophisticated technology-driven approaches can not only root out fraud, but find it before payment is made. Whether it is contract fraud or Medicaid fraud, the undertaking of a criminal ring or the efforts of a sole, dedicated fraudster – fraud is not only findable, it’s preventable.
The key is to move from a reactive to a proactive approach. Almost all efforts to combat government fraud are reactive in nature – an investigator finds something suspicious, or the agency overseeing the contract spots illegal activity, or a tip comes in. By that point the payment has already been made and investigators are left to chase after the money. Just like prevention is the key to staying healthy, a proactive approach can reduce the 5 to 7 percent of government dollars that end up in fraudsters’ pockets.
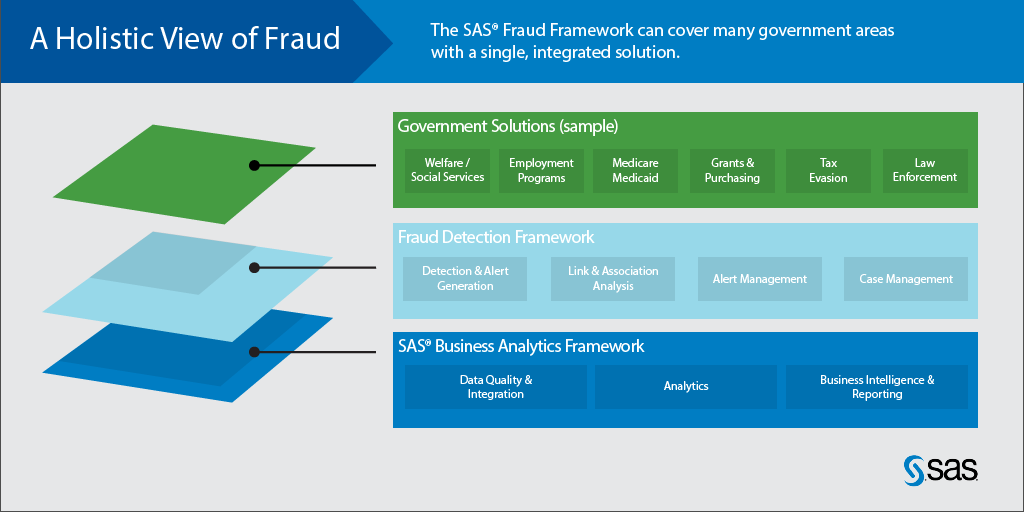
A hybrid approach
When you have full data integration and pair it with anomaly detection, robust social network analysis and predictive capabilities you’ve got a system for fighting fraud that is much more potent than individual efforts. To understand this technology’s potential in rewriting the “pay and chase” model, you need to understand its three components:
Improved data integration: You need to be able to bring data together data from a wide variety of third-party data sources and combine it with federal agency data on a national level to better battle food stamp, Small Business Administration and other forms of government fraud. Being able to check for missing and non-standard data quickly is critical, as is weaving in unstructured data from call centers or investigator notes. With this approach, it’s easier to spot deceased loan recipients, incarcerated beneficiaries, false storefronts and inappropriate addresses (a medical clinic with a UPS store address). Learn more about the role of data integration.
Robust social network analysis: Government benefit programs are ripe targets for fraudsters. The trail they leave can often be sniffed by anomaly detection – such as the case of the convenience store in the food stamp program that had a $104.75 transaction average vs. the $5.50 average. But anomaly detection alone simply sets up the chase. To stop payments before they are made, you need social network analysis. By automating the review of ownership filings, tax records and similar data, government agencies can spot the friends and families likely engaged in similar activities and stop payment while the pattern is further investigated. In the case above, investigators ultimately found four related convenience stores that were involved in a $1.6 million collusive scam. Read more in this paper.
Predictive capabilities: A crime ring that stole physician information and created phony clinics bilked federal payers for more than $100 million because their sophisticated efforts easily outran alert thresholds designed to root out these kinds of fraud. When predictive analytics is paired with anomaly detection, you can build models that use information learned from previous frauds to detect new ones. Learn more about how predictive analytics and other sophisticated techniques can take down medical payment fraudsters.
The volume of data in so many government programs makes vigilantly fighting fraud critical. To learn more about the technologies visit the government solutions site on our website.

Read More
The volume of data managed in so many government programs makes vigilantly fighting fraud critical. To learn more about the technologies visit the government solutions site on our website.
Get More Insights
Want more Insights from SAS? Subscribe to our Insights newsletter. Or check back often to get more insights on the topics you care about, including analytics, big data, data management, marketing, and risk & fraud.
